Watching your child struggle to breathe during an asthma attack is every parent’s nightmare. In 2026, that fear is being transformed into proactive confidence thanks to revolutionary smart inhaler sensor technology that turns ordinary rescue and controller inhalers into intelligent health companions. These tiny, sophisticated devices don’t just track medication usage—they create a comprehensive digital safety net that grows with your child, providing peace of mind for families while empowering young patients to take ownership of their respiratory health.
But with a rapidly expanding market of pediatric-focused sensors, each promising to be the ultimate solution, how do you cut through the noise? This guide walks you through everything you need to know about selecting the right smart inhaler sensor for your child, from clinical validation requirements to gamification features that actually work, ensuring your investment translates into real-world asthma control and fewer midnight trips to the emergency room.
Top 10 Smart Inhaler Sensors for Pediatric Asthma
Detailed Product Reviews
1. “Asthma Inhaler Inside” Alert Tags. Double Sided Medical Tags (two piece set)

Overview: These medical alert tags provide critical visibility for asthma sufferers, featuring a clear “Asthma Inhaler Inside” message on both sides. Constructed from solid, one-piece metal with a protective coating, this two-piece set attaches to backpacks, purses, key chains, or luggage using included clips. The durable design resists scratches and dirt while ensuring emergency personnel can quickly identify your condition and medication location.
What Makes It Stand Out: The double-sided messaging is a crucial safety feature, eliminating the risk of the tag flipping over and becoming unreadable during an emergency. Unlike plastic alternatives, the metal construction provides exceptional durability for daily wear and tear. The versatile clip system allows simultaneous attachment to multiple items, creating redundant alerts for your inhaler’s location. The scratch-resistant coating maintains legibility long after cheaper tags would fade.
Value for Money: At $9.99 for a two-piece set, these tags represent excellent value compared to custom-engraved medical IDs that often cost $15-25 each. The robust metal construction ensures years of use, making the per-year cost negligible. While they don’t provide physical protection like a case, they serve a distinct and vital purpose that could prove life-saving during a severe asthma attack when every second counts.
Strengths and Weaknesses: Pros: Double-sided alert maximizes visibility; durable metal construction outlasts plastic alternatives; includes versatile attachment clips; scratch-resistant coating maintains readability; lightweight and unobtrusive. Cons: Tags only—no protective case included; metal may scratch other items in pockets or bags; limited space for additional medical information beyond asthma alert.
Bottom Line: These alert tags are an essential, cost-effective safety addition for anyone with asthma, especially children at school or active adults. Pair them with a protective case for complete peace of mind. The durable construction and double-sided design make them superior to most medical tags under $15.
2. Asthma Inhaler Portable Case for Adults, Kids & Seniors - Multi-Zone Lining for Inhaler/Spacer/Emergency Meds, Waterproof PU & Travel-Ready with Mesh Pocket,Black (Only Case)
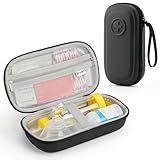
Overview: This versatile black PU case offers comprehensive storage for asthma management tools, accommodating inhalers, spacers, emergency medications, and small accessories. Designed for all ages with rounded edges and a wide opening, the waterproof construction features multi-zone compartments and a wrist strap for convenient transport. The smart organization includes a zippered mesh pocket in the upper lid and elastic straps in the lower section to secure devices.
What Makes It Stand Out: The multi-zone lining system is exceptionally well-designed, creating distinct spaces for medications and equipment while protecting them from moisture, dust, and temperature fluctuations. The waterproof PU fabric paired with mesh pockets offers superior environmental protection compared to standard fabric cases. The thoughtful inclusion of an emergency contact card adds a layer of safety, while the wrist strap provides hands-free carrying without needing a carabiner.
Value for Money: Priced at $14.99, this case delivers premium features typically found in $20+ competitors. The waterproof PU material and intelligent compartmentalization justify the cost, offering protection that could prevent medication spoilage. While EVA hard shells provide more impact resistance, this case’s softer construction allows it to fit more bag types and absorb shock differently, making it ideal for daily commuting and school use.
Strengths and Weaknesses: Pros: Excellent multi-zone organization prevents clutter; waterproof PU fabric protects against moisture; all-age design with safety-rounded edges; includes wrist strap and emergency card; lightweight and highly portable. Cons: PU material offers less impact protection than hard EVA; may not fit larger spacers or multiple inhalers; black color lacks high-visibility emergency identification.
Bottom Line: This case excels for daily use, school, and travel where organization and moisture protection are priorities. The smart storage design makes it perfect for managing complex medication regimens. Choose this over basic pouches for its superior protection and thoughtful compartmentalization at a competitive price point.
3. MGZNMTY Travel Carrying Case Compatible with Asthma Inhaler Spacer for Adults and Children, Masks, Inhaler Holder with Asthma Alert Tag and Medical Card, Carabiner (Only Case) (Galaxy)

Overview: This galaxy-patterned EVA case provides robust protection for complete asthma kits, including inhalers, spacers, masks, and emergency medications like EpiPens. The semi-waterproof, shockproof, dustproof construction features built-in elastic straps and mesh pockets, plus an included asthma alert tag and emergency medical ID card. Exterior dimensions of 9.1" x 4.7" x 2.8" offer substantial capacity while remaining portable with a hand strap and carabiner.
What Makes It Stand Out: The comprehensive accessory package sets this apart—most cases force you to purchase alert tags and medical cards separately. The hard EVA shell provides superior impact protection compared to fabric cases, while the galaxy design makes it visually appealing for children and teens who might otherwise resist carrying medical equipment. The inclusion of both hand strap and carabiner offers unmatched versatility for school, travel, or outdoor activities.
Value for Money: At $16.99, this represents exceptional value. Purchasing a comparable hard EVA case ($12-15), metal alert tag ($5-10), and medical ID card ($3-5) separately would cost $20-30. The shockproof construction could prevent hundreds of dollars in damaged equipment, while the included safety documentation provides peace of mind. The slightly higher price over basic cases is justified by the complete protection and accessory bundle.
Strengths and Weaknesses: Pros: Hard EVA shell offers maximum protection; includes alert tag and medical card; versatile carry options (strap and carabiner); spacious interior fits spacers and masks; appealing galaxy pattern encourages use. Cons: Pattern may not suit professional adult environments; larger size may be bulky for small purses; elastic straps may stretch over time with heavy spacers.
Bottom Line: This is the best all-in-one solution for families seeking maximum protection and complete emergency preparedness. The hard shell and included accessories make it ideal for children, active teens, and travelers. The galaxy design specifically helps with compliance in younger users. Highly recommended as a comprehensive asthma management system.
4. e-Pill Asthma Inhaler & Peak Flow Meter Travel Case – Medical Storage Organizer for Home, School & Travel (No Inhaler Included)

Overview: The e-Pill case is specifically designed to accommodate both asthma inhalers and peak flow meters, making it unique among carriers. The bright red color ensures high visibility in emergencies, while the compact, lightweight design features durable construction and a clip-on carabiner. This case protects equipment from dust, debris, and damage during daily use or travel, with an easy-open design for quick medication access when seconds matter.
What Makes It Stand Out: The dedicated peak flow meter storage distinguishes this from universal cases, providing a tailored solution for patients who monitor lung function regularly. The bright red color serves as both a visual alert and a location beacon in cluttered bags—a critical feature during emergencies. The e-Pill brand carries medical device credibility, and the case’s design reflects clinical utility over generic storage. The carabiner attachment is robust and positioned for secure bag mounting.
Value for Money: At $24.95, this is a premium-priced option. The cost is justified for patients requiring peak flow meter portability, as alternative solutions often involve carrying separate cases. For users only needing inhaler storage, however, the price is high compared to $15-18 alternatives with similar protection. The medical-grade branding and specialized design command a 40% premium over generic cases, which may be worth it for school nurses or clinical settings.
Strengths and Weaknesses: Pros: Accommodates peak flow meters and inhalers; high-visibility red color aids emergency location; trusted medical brand; durable construction; carabiner included; easy-access design. Cons: Significantly more expensive than competitors; no included medical alert tag or ID card; red color may be too conspicuous for some users; limited internal organization features.
Bottom Line: This case is ideal for patients who regularly use peak flow meters and need clinical-grade organization. The red color and brand credibility make it perfect for school health offices and elderly users. However, those only carrying inhalers will find better value elsewhere. Choose this for its specific capacity and medical professionalism, not as a general-purpose case.
5. CASEMATIX Asthma Inhaler Case Protects Asthma Holder From Accidental Sprays and Dirt, Includes Blue Green Case Only

Overview: The CASEMATIX case features an ultra-compact L-shaped molded design in blue with a green zipper, tailored specifically for inhaler protection. Measuring just 4.5" x 2.0" x 2.0", this hard-shell EVA case with leatherized rubber lining prevents accidental activation and shields against dirt and damage. It includes a heavy-duty zipper, removable carabiner, belt loop, and lanyard for multiple carry options, making it exceptionally portable for everyday use, hiking, or school.
What Makes It Stand Out: The L-shaped molding is ingeniously space-efficient, creating a form-fitting profile that eliminates wasted space while providing hard-shell protection. The inclusion of three distinct carry systems—carabiner, belt loop, AND lanyard—is unmatched at this price point, offering users complete flexibility in how they keep their inhaler accessible. The leatherized rubber interior provides a premium feel and superior grip compared to standard fabric linings, preventing the inhaler from shifting during activity.
Value for Money: At $14.99, this case delivers exceptional value for active users. The hard EVA construction typically commands $18-25 from competitors, and the triple-carry system would cost $5-10 to replicate separately. The compact design’s efficiency means it fits virtually anywhere, potentially replacing larger, more expensive cases. For hikers, students, and athletes who need instant, reliable access, the durability and versatility justify every penny.
Strengths and Weaknesses: Pros: Ultra-compact L-shaped design saves space; hard EVA shell prevents accidental sprays; three carry options (carabiner, belt, lanyard); durable heavy-duty zipper; premium interior lining; highly portable. Cons: Extremely limited storage—fits inhaler only, no spacers or meds; L-shape may not accommodate all inhaler models; no included medical alert documentation; small size makes it easy to misplace.
Bottom Line: This is the ultimate minimalist case for active individuals who prioritize portability and instant access above all else. The hard-shell protection and multiple carry options make it perfect for sports, hiking, and school use. However, those needing to carry spacers or multiple medications will find it too limiting. For single-inhaler users seeking maximum portability and protection, this is the best choice under $15.
6. VdLis – EVA Hard Shell Asthma Inhaler Case & Inhaler Spacer Organizer | Portable Nebulizer Case & Inhaler Holder with Unicorn Design – Washable Medical Storage

Overview: The VdLis EVA Hard Shell Asthma Inhaler Case transforms pediatric asthma management with its whimsical unicorn design. This 22×12×7 cm portable organizer protects inhalers, spacers, and compact nebulizers while making daily medication routines less intimidating for children. The case fits easily into school bags and travel kits, providing a protective barrier against bumps and scratches that active kids inevitably encounter. Its machine-washable construction ensures hygienic storage, addressing parents’ concerns about keeping medical equipment clean.
What Makes It Stand Out: The magical unicorn motif directly tackles psychological barriers to pediatric asthma compliance, turning medical necessity into something children willingly carry. Unlike generic cases, the EVA hard shell provides genuine impact protection for expensive equipment, while the 30°C machine-washable feature maintains clinical cleanliness without complicated care routines. The smooth zipper operation empowers children to access their medication independently, building confidence and self-management skills. This combination of emotional appeal and practical protection creates a unique value proposition in pediatric medical accessories.
Value for Money: At $12.99, this case delivers exceptional value for parents struggling with medication adherence. Comparable children’s medical cases typically cost $15-25 yet rarely offer the same trifecta of engaging design, robust protection, and washable convenience. The potential improvement in daily compliance alone justifies the investment, while the durable construction ensures longevity through years of school and activities. For budget-conscious families, it eliminates the need to choose between affordability and child-friendly design.
Strengths and Weaknesses: Strengths include the engaging unicorn aesthetic that reduces anxiety and encourages compliance, durable EVA protection against drops, compact travel-friendly dimensions, machine-washable hygiene maintenance, and independent zipper access for children. The affordable price point makes it accessible. Weaknesses include the child-specific design that may not suit older kids, limited interior organization beyond main compartment, and potential size constraints for larger spacer models. Parents should verify device compatibility, as the unicorn theme may also not appeal to all children.
Bottom Line: This case is a strategic purchase for parents of young children with asthma who face resistance to medication routines. The unicorn design effectively reduces stigma while the protective, washable construction ensures durability and hygiene. For under $13, it delivers both practical functionality and emotional support in pediatric asthma management.
7. CASEMATIX Asthma Inhaler Case Fits Inhaler Spacer For Adults, Masks, Inhaler Holder and More - Compact Size Fits 6.25" Maximum, Includes CASE ONLY

Overview: The CASEMATIX Asthma Inhaler Case delivers adult-focused functionality in a rugged 7.0" x 4.0" x 2.5" hard-shell design. It accommodates inhalers, spacers up to 6.25 inches, Epipens, and face masks, making it a versatile medical equipment organizer. The insulated Myler interior creates a sanitary, easy-to-clean environment, while the exterior features prominent medical identification elements. A carabiner clip and included keychain provide versatile attachment options for active adults who need reliable access to their medication.
What Makes It Stand Out: The integrated medical alert system distinguishes this case with both an exterior medical cross and an “I Have ASTHMA” first aid keychain, communicating critical information during emergencies. The insulated Myler interior is a premium feature rarely found in this category, offering superior cleanliness and protection against temperature fluctuations. The carabiner enables secure attachment to backpacks, gym bags, or belt loops, ensuring the inhaler remains accessible during various activities without risk of loss.
Value for Money: At $18.99, this case commands a mid-range price justified by specialized medical features and durable construction. While basic EVA cases sell for $12-15, the added value of Myler insulation, dual medical alert system, and carabiner attachment represents a worthwhile premium for adults prioritizing emergency preparedness and professional-grade protection. The investment pays dividends in equipment longevity and peace of mind, particularly for those with severe asthma requiring immediate device access.
Strengths and Weaknesses: Strengths include the effective medical alert system for emergencies, insulated Myler interior for hygiene and temperature control, durable EVA hard shell protection, versatile carabiner attachment, and compact portability fitting various accessories. The case serves multiple device types. Weaknesses include the 6.25" length limitation excluding some larger spacers, lack of interior organization pockets, higher price than basic alternatives, and utilitarian aesthetic that may not appeal to younger users. The “case only” limitation requires separate accessory purchases.
Bottom Line: This case is ideal for adults seeking a professional, safety-conscious solution for asthma management on the go. The medical alert features and insulated interior justify the moderate price premium. Verify your spacer length before purchasing, but for those prioritizing emergency preparedness and hygiene, this case delivers exceptional functional value.
8. Elonbo Carrying Case for Asthma Inhaler, Inhaler Spacer for Kids and Adults, Masks, Inhaler Holder Asthma Travel Organize Bag, Pocket Fits Allergy Meds, Ventolin Inhaler, Black (Case Only)

Overview: The Elonbo Carrying Case offers universal asthma equipment storage for both children and adults in a sleek black design. This versatile organizer accommodates inhalers, spacers for all ages, masks, Ventolin inhalers, allergy medications, and even oximeters. Constructed with PU leather-reinforced EVA hard shell and soft interior lining, it provides comprehensive protection against shocks, water, dust, and static electricity. The thoughtful interior includes elastic straps and a mesh pocket for organized storage, making it a practical solution for families managing multiple respiratory conditions.
What Makes It Stand Out: The universal design philosophy eliminates age-based purchasing decisions, making it suitable for families with multiple asthma sufferers. The dual zipper configuration provides flexible access from either side, while the elastic securing straps prevent equipment from shifting during movement—a critical feature for protecting sensitive medical devices. The comfortable built-in handle transforms it from a simple case into a portable medical kit, enhancing its utility for travel, school, and outdoor activities where quick access matters.
Value for Money: Priced at $14.99, this case strikes an excellent balance between premium features and affordability. It undercuts many adult-focused competitors while offering superior interior organization through its mesh pocket and elastic straps. Comparable cases with similar protection levels and organizational features typically retail for $18-22. The universal sizing for both pediatric and adult equipment adds family value, potentially eliminating the need for separate cases and making it a cost-effective household solution.
Strengths and Weaknesses: Strengths include universal design for all ages, superior interior organization with mesh pocket and elastic straps, comprehensive protection (shockproof, waterproof, dustproof), comfortable carry handle, double zipper convenience, and competitive pricing. The neutral black aesthetic suits various preferences. Weaknesses include lack of medical alert identification, no insulation for temperature control, and potential size limitations for larger nebulizer units. The “case only” nature requires separate accessory procurement, and the black color may be easily lost in bags.
Bottom Line: This case is an outstanding choice for families seeking a versatile, well-organized solution for asthma equipment storage. The universal design, protective features, and interior organization provide exceptional value at $14.99. While it lacks emergency identification features, its functional design and durability make it a practical investment for daily use and travel across all age groups.
9. YouKnow Travel Carrying Case for Asthma Inhaler, Inhaler Spacer for Adults and Children, Mask, Inhaler Holder with Asthma Warning Label and Medical Card, with Carabiner (Case Only) (Galaxy)

Overview: The YouKnow Travel Carrying Case merges style with emergency preparedness in a galaxy-themed design suitable for all ages. This case accommodates inhaler spacers, masks, and related accessories for both adults and children, with outer dimensions of 9.1" x 4.7" x 2.8". The package includes vital safety features: an “I Have Asthma - Inside Inhaler” warning label and a comprehensive emergency medical ID card for documenting critical health information. The addition of a shoulder strap and carabiner provides versatile portability options for active lifestyles.
What Makes It Stand Out: The integrated emergency medical ID card system is a standout safety feature, allowing users to document medications, allergies, and conditions for first responders. This proactive approach to emergency preparedness exceeds standard case functionality. The galaxy design appeals to younger users while remaining stylish enough for adults, bridging the age gap that often segments asthma products. The shoulder strap offers hands-free convenience unavailable in many competing cases, making it ideal for active lifestyles where bags may not be practical.
Value for Money: At $16.99, this case delivers strong value through its combination of safety documentation, versatile carrying options, and appealing aesthetics. While priced slightly above basic cases, the emergency ID system alone justifies the premium. Similar medical alert accessories purchased separately would cost $5-10, making this an integrated value proposition. The customer satisfaction guarantee provides additional purchase confidence, reducing risk for buyers uncertain about sizing or quality.
Strengths and Weaknesses: Strengths include the comprehensive emergency medical ID card system, stylish galaxy design for broad age appeal, dual carrying options (shoulder strap and carabiner), clear asthma warning label, and customer satisfaction guarantee. The case accommodates various device sizes and portable nebulizers. Weaknesses include no interior organization features mentioned, lack of insulation or specialized medical-grade interior, potential size bulkiness for smaller bags, and absence of interior securing straps. The galaxy pattern may not suit professional environments.
Bottom Line: This case excels for users prioritizing emergency preparedness and style versatility. The medical ID system and multiple carrying options make it ideal for active children and adults alike. At $16.99, it offers integrated safety features that justify the moderate price. While lacking advanced interior organization, its emergency documentation capabilities make it a smart choice for peace of mind.
10. Vivélle Carrying Case for Portable Handheld Inhaler Nebulizer Machine for Adults and Kids, Asthma Inhaler Travel Case, Handheld Mesh Atomizer Machine Holder, Inhaler Spacer Bag. Case Only

Overview: The Vivélle Carrying Case specializes in protecting portable handheld nebulizer machines and inhaler spacers for both adults and children. Precision-molded to fit most rechargeable mesh nebulizer models, this case also accommodates asthma inhaler spacers and insulin pens, making it versatile for users with multiple respiratory or diabetic needs. Constructed with durable PU leather-reinforced EVA hard shell and soft interior lining, it provides travel-ready protection against drops, dust, water, and static. The organized interior features elastic straps and a mesh pocket for accessories.
What Makes It Stand Out: The case’s specific design for handheld nebulizer machines fills a niche gap, as most cases only accommodate inhalers and spacers. This specialization ensures a secure fit for expensive nebulizer equipment that requires superior protection for sensitive mesh atomizer components. Its versatility across asthma and diabetes management equipment makes it valuable for users with comorbid conditions, eliminating the need for separate storage solutions. The precision molding prevents device movement that could damage delicate electronic components during travel.
Value for Money: At $18.00, this case positions itself in the premium segment, justified by specialized nebulizer protection and multi-condition versatility. Standard inhaler cases retail for $12-16 but lack the tailored fit for nebulizer machines costing $50-200. The potential cost savings from preventing device damage makes this a wise insurance policy. For users requiring both asthma and diabetic supplies, the dual functionality eliminates a second purchase, enhancing overall value despite the higher initial investment.
Strengths and Weaknesses: Strengths include specialized design for handheld nebulizer machines, versatile accommodation of inhalers and insulin pens, heavy-duty protection with PU leather reinforcement, organized interior with straps and pocket, lightweight portability, and convenient carry handle. The case serves multiple medical conditions effectively. Weaknesses include higher price point, potential over-sizing for users with only inhalers, limited aesthetic options, and unspecified maximum device dimensions requiring verification. The premium features may exceed needs for basic inhaler storage alone.
Bottom Line: This case is essential for users of portable handheld nebulizers who need specialized protection for sensitive equipment. The $18.00 investment safeguards significantly more expensive devices while offering versatility for other medical supplies. For those managing multiple conditions or relying on nebulizer therapy, this case provides unmatched specialized protection and organizational value.
The Evolution of Pediatric Asthma Care in 2026
Pediatric asthma management has undergone a seismic shift from reactive crisis treatment to predictive, data-driven prevention. Connected inhaler sensors represent the convergence of pediatric pulmonology, digital therapeutics, and child psychology, creating tools that speak to both clinical needs and developmental stages. Unlike adult-focused devices retrofitted for children, 2026’s generation of sensors are purpose-built for growing bodies, varying cognitive abilities, and the unique rhythms of family life.
Why Smart Sensors Are Game-Changers for Children
Children face distinct challenges in asthma management: inconsistent technique, difficulty recognizing symptoms, and reliance on caregivers who can’t be present 24/7. Smart sensors address these gaps by providing objective usage data that eliminates the guesswork from parent reports. They capture critical information like inspiratory flow rate, which directly impacts medication deposition in small airways—a factor particularly crucial in pediatric patients whose lung development varies dramatically by age. This data transforms vague “I think he used it” into actionable insights about whether your child actually received a therapeutic dose.
Traditional vs. Connected Inhaler Therapy
The old paradigm relied on manual peak flow meters, paper symptom diaries (often incomplete), and retrospective recall during quarterly appointments. Smart sensors create a continuous feedback loop, alerting you to patterns invisible to the naked eye: the Tuesday spike in rescue inhaler use that correlates with gym class, the declining technique quality that precedes exacerbations, or the forgotten evening doses that derail control. For pediatric patients, this means interventions happen in real-time rather than after weeks of silent deterioration.
Understanding Smart Inhaler Sensor Technology
Before diving into features, understanding the underlying technology helps you evaluate claims and avoid marketing hype. Modern sensors are marvels of miniaturization, packing accelerometers, pressure sensors, and environmental detectors into units weighing less than a sugar packet.
How Sensors Attach to Existing Inhalers
Attachment mechanisms vary significantly and impact daily usability. Cap-based sensors replace the standard inhaler mouthpiece cover, offering seamless integration but requiring replacement when the inhaler itself is swapped. Clip-on devices fasten to the inhaler’s body, providing transferability between devices but potentially interfering with grip for small hands. Adhesive-mounted options offer universal compatibility but raise concerns about residue and precise positioning. For pediatric use, consider your child’s dexterity and whether they’ll be transitioning between multiple inhalers (school vs. home).
Core Biometric and Environmental Tracking Capabilities
Beyond simple dose counting, advanced sensors now measure inspiratory flow profiles to assess technique quality—critical for children who often inhale too rapidly or insufficiently. Environmental sensors detect temperature, humidity, and airborne particulates, correlating symptoms with triggers like pollen, pollution, or classroom air quality. Some platforms integrate with wearable chest sensors to capture respiratory rate and wheeze detection, creating a multi-dimensional view of your child’s respiratory status that goes far beyond medication adherence alone.
Data Transmission Methods: Bluetooth, NFC, and Beyond
Bluetooth Low Energy (BLE) remains the standard for real-time syncing, but its constant connectivity drains smartphone batteries and raises school privacy concerns. NFC (Near Field Communication) requires deliberate tap-to-sync actions, which can be a feature rather than a bug for privacy-conscious families. Emerging ultra-wideband (UWB) technology enables passive background syncing without battery penalty, while some sensors now offer optional LTE-M connectivity for children without smartphones, transmitting directly to parental dashboards. Consider your child’s school technology policies and your family’s device ecosystem when evaluating transmission protocols.
Key Features That Matter for Pediatric Patients
Not all sensor features translate equally to pediatric success. The best devices prioritize developmental appropriateness over technical specifications.
Age-Appropriate Design and Durability
Toddlers require rugged, droppable sensors with no small parts, while teenagers demand discreet, aesthetically pleasing devices that don’t scream “medical equipment.” Look for IP67+ water resistance ratings—because inhalers inevitably end up in backpacks with leaking water bottles. Drop-test certifications from 1.5 meters simulate real-world playground accidents. For younger children, sensors with rounded edges and chew-resistant materials prevent safety hazards, while glow-in-the-dark or tactile features help visually impaired or developmentally delayed patients locate their devices.
Gamification Elements That Actually Work
Beware of superficial badge systems that lose appeal after two weeks. Effective pediatric gamification ties directly to clinical outcomes: points for proper technique (not just usage), streaks for adherence, and character progression that unlocks when asthma control improves. The most successful platforms use collaborative challenges where parents and children work together toward shared goals, reducing adversarial dynamics around medication time. Look for evidence-based behavior change frameworks like self-determination theory baked into the reward architecture, not just colorful graphics.
Real-Time Medication Reminders for Busy Families
Generic “time for your inhaler” alerts create notification fatigue. Sophisticated systems use geofencing to remind children at school without bothering them at home, or predictive timing based on your child’s actual usage patterns rather than rigid schedules. Parental escalation features—where unanswered child reminders trigger parent notifications after a grace period—prevent caregiver burnout while ensuring nothing falls through the cracks. The ability to customize reminder tones with your child’s favorite song or a reassuring parent’s voice message transforms a clinical alert into a comforting routine.
Multi-User Support for School and Home Environments
Your child’s inhaler sensor must seamlessly transition between home, school, and other caregivers without data loss or privacy breaches. Look for role-based access controls that let school nurses view usage but not historical trends, while giving parents full access. Temporary caregiver modes for babysitters or grandparents provide limited functionality without compromising primary account security. The best systems automatically detect which inhaler is being used (school rescue vs. home controller) and attribute data appropriately, even when children carry multiple devices.
Clinical Validation and FDA Approvals
In the rush to market, not all sensors undergo rigorous pediatric testing. Understanding validation levels protects your family from investing in digital snake oil.
What “Clinically Validated” Means for Your Child
True clinical validation requires peer-reviewed studies specifically including pediatric subjects—not just adult data extrapolated downward. Look for publications demonstrating improved asthma control scores (cACT), reduced exacerbations, or validated correlation with spirometry in children aged 4-17. The gold standard includes prospective, randomized controlled trials showing sensor use leads to clinically meaningful outcomes, not just improved adherence metrics. Be wary of “clinically tested” claims without published methodology; this often means a single pilot study with a dozen adult participants.
Understanding Regulatory Pathways in 2026
The FDA’s 2023 Digital Health Policy modernized oversight, creating distinct pathways for pediatric digital therapeutics. Sensors with algorithmic features (like exacerbation prediction) require 510(k) clearance or De Novo classification as Software as a Medical Device (SaMD). Those claiming to diagnose or treat require full premarket approval. Check the FDA’s Digital Health Technologies database for your device’s classification and any pediatric-specific labeling. European CE marking under MDR (Medical Device Regulation) also provides assurance, but verify the notified body included pediatric experts in their review.
The Role of Peer-Reviewed Studies in Sensor Selection
Prioritize devices with published pediatric data in journals like Pediatric Pulmonology or the Journal of Allergy and Clinical Immunology. Studies should report on age-stratified outcomes, as a sensor effective for teenagers may fail for preschoolers. Look for real-world evidence (RWE) studies beyond controlled trials—data from thousands of actual pediatric users in everyday settings provides more relevant insights than pristine clinical environments. Manufacturer partnerships with children’s hospitals for ongoing research indicates commitment to pediatric-specific optimization.
Integration with Pediatric Healthcare Ecosystems
A sensor that creates data siloes wastes everyone’s time. Seamless integration transforms raw metrics into collaborative care.
EHR Compatibility and Pediatrician Dashboards
Your pediatrician’s time is limited; sensors that auto-populate electronic health records with structured data (not PDF reports) enable efficient review during appointments. Look for HL7 FHIR compliance and direct integration with major pediatric EHRs like Epic MyChart or Cerner PowerChart. The best platforms provide clinicians with pediatric-specific dashboards highlighting concerning trends without overwhelming them with raw data. Ask your pulmonologist which platforms they can actually access—some “integrated” systems require manual data export that never happens in practice.
School Nurse Portal Access and Privacy Considerations
School integration requires delicate privacy balancing. HIPAA doesn’t apply directly to schools, but FERPA does. Opt for platforms offering BAA (Business Associate Agreement) compliant school portals that limit data collection to what’s medically necessary. Time-limited access that automatically expires at school year-end prevents permanent data retention by educational institutions. Critical features include one-click asthma action plan access for nurses and emergency contact escalation, but avoid systems that share detailed trend data with non-medical school staff.
Parental Control vs. Child Independence Features
The sensor journey should evolve as your child matures. For ages 4-8, parental dashboards should offer complete control with simplified child interfaces. Ages 9-12 benefit from shared dashboards where children can view (but not edit) their data, fostering responsibility. Teenagers require privacy partitions—parents receive adherence summaries and emergency alerts, while teens access detailed analytics and self-management tools. Look for graduated control settings that transition smoothly, preventing the sudden “handoff” that can cause adherence drops during adolescence.
Data Privacy and Security for Young Patients
Children’s health data is a prime target for breaches and exploitation. Security features must be non-negotiable.
HIPAA Compliance and COPPA Protections
Any pediatric sensor must be HIPAA-compliant, but COPPA (Children’s Online Privacy Protection Act) adds crucial layers. Verify the manufacturer doesn’t sell data to third parties—a surprising number of “free” apps monetize pediatric health information. Look for explicit statements that data is not used for advertising or insurance underwriting. The best platforms undergo regular third-party security audits and publish results. For children under 13, parental consent should be required for any data sharing, even anonymized aggregation.
Data Ownership in Pediatric Healthcare
Read the terms of service carefully: who owns your child’s data? Ethical platforms grant families full ownership with the right to export or delete all information. Avoid services that claim perpetual licenses to use pediatric data for “research” without explicit opt-in for each study. Some platforms now offer data escrow arrangements where information is held by a neutral third party, preventing manufacturer lock-in and ensuring access even if the company ceases operations.
Secure Family Sharing Architectures
Multi-generational caregiver access creates security vulnerabilities. Look for end-to-end encryption where only family members with cryptographic keys can view data, not even the manufacturer. Two-factor authentication should be mandatory, not optional. Consider platforms using zero-knowledge architecture, where decrypted data never touches manufacturer servers. For divorced or separated families, granular access controls that comply with custody agreements prevent conflict while ensuring both parents receive emergency notifications.
Battery Life, Maintenance, and Sustainability
A dead sensor provides no protection. Pediatric-specific usage patterns demand robust power management.
Longevity Expectations for Daily Pediatric Use
Most sensors promise 6-12 months, but children’s frequent usage and accidental button presses drain batteries faster. Seek devices with 18+ month battery life or rechargeable options with wireless charging pads that become part of the nightly routine. Solar-assisted charging cases offer eco-friendly power for forgetful teens. Critical: sensors should continue collecting data even when the battery is critically low, syncing later rather than dying mid-day and losing precious information.
Eco-Friendly Materials and Recycling Programs
Children’s environmental consciousness is rising, and sensors should reflect family values. Look for medical-grade bioplastics derived from renewable sources, not petroleum-based polymers. Manufacturers offering take-back programs for responsible battery disposal and sensor recycling demonstrate long-term commitment. Some platforms now include carbon offset credits in their subscription, appealing to environmentally aware families. For younger children, BPA-free and phthalate-free certifications are non-negotiable given the tendency to mouth objects.
Warranty and Replacement Policies
Pediatric use voids many standard warranties. Seek manufacturers offering “kid-proof” warranties covering accidental damage, loss, and even theft at school. Lifetime sensor replacement programs with modest monthly subscriptions often cost less than replacing devices out-of-pocket. Check if replacements are expedited—asthma can’t wait for standard shipping. Some platforms offer “hot swap” programs where a replacement arrives before you return the broken unit, ensuring continuous coverage.
Insurance Coverage and Accessibility in 2026
The best sensor is worthless if you can’t afford it. Navigating reimbursement remains complex but improving.
Navigating Payer Reimbursement Landscapes
As of 2026, most commercial insurers cover smart sensors as Durable Medical Equipment (DME) when prescribed with documented poor adherence or frequent exacerbations. Prior authorization is typically required, so involve your pediatrician early. CPT codes 99091 and 99457 (remote patient monitoring) may cover associated data review services. Some sensors are now bundled with inhaler medications, appearing as a single co-pay. Always appeal denials—many insurers initially reject claims that should be covered under pediatric chronic disease management programs.
Medicaid and CHIP Considerations
Coverage varies dramatically by state, but Medicaid expansion of digital health benefits has accelerated. Many state programs now cover sensors for children with severe persistent asthma or those in high-risk zip codes. CHIP (Children’s Health Insurance Program) coverage is improving but often requires demonstration of cost-effectiveness. Manufacturer Medicaid-specific programs may provide sensors at no cost while reimbursement is pending. Contact your state’s Medicaid pharmacy benefit manager directly—coverage decisions are often made at that level and may not be reflected in general policy documents.
Manufacturer Assistance Programs
Most manufacturers offer sliding-scale assistance programs based on household income, with some providing free sensors to families under 200% of federal poverty level. Manufacturer-sponsored “bridge programs” supply sensors during insurance approval delays, typically 30-90 days. Beware of programs that require switching pharmacies or medications—the best assistance is device-agnostic. Some platforms now offer “success-based pricing” where you pay only if adherence improves, aligning manufacturer incentives with your child’s outcomes.
Setting Up Your Child’s Smart Inhaler System
Even the best sensor fails with poor onboarding. A systematic approach ensures adoption rather than abandonment.
Step-by-Step Onboarding for Families
Start with a “sensor ceremony” where your child personalizes their device with stickers or color choices, building ownership. Pair the sensor during a calm moment, not during an asthma flare. Practice technique with the sensor’s real-time feedback feature—many children need 5-10 supervised attempts before achieving correct inspiratory flow. Set up caregiver accounts before the child’s account, establishing the support network. Most importantly, integrate sensor checks into existing routines: morning teeth brushing, backpack packing, or bedtime stories.
Troubleshooting Common Connectivity Issues
School Wi-Fi networks often block medical device traffic. Pre-configure sensors to sync via cellular backup during school hours. Bluetooth interference from other devices is common; teach children to hold their inhaler away from other electronics during syncing. For sensors that lose time stamps, manually logging events in the app for 48 hours often recalibrates internal clocks. If data seems inaccurate, check that the sensor is oriented correctly—upside-down mounting is a frequent pediatric issue given how children grab inhalers.
Calibrating Sensors for Pediatric Dosing
Standard sensors calibrate for adult inhaler actuation force, but children generate less pressure. Look for pediatric calibration modes that adjust sensitivity for lower-force actuations common in kids under 12. Some sensors require manual calibration using a placebo inhaler—complete this process with your child using their actual technique, not an adult’s. Recalibrate every time you change inhaler brands, as canister resistance varies. For breath-actuated inhalers, verify the sensor can distinguish between device-triggered and manual actuations to prevent false positives.
Measuring Success: Metrics That Matter
Raw adherence percentages mislead. Pediatric success requires nuanced metrics aligned with developmental goals.
Beyond Adherence: Quality of Inhalation Technique
The best platforms score each inhalation on flow rate, duration, and breath-hold, providing technique quality scores that predict medication efficacy. Look for age-normed benchmarks—a “good” inhalation for a 5-year-old differs from a 15-year-old. Sensors that detect exhalation into the device (a common pediatric error) provide immediate corrective feedback, preventing wasted doses. Track technique improvement trends over months, celebrating when your child masters proper inhalation rather than just remembering to use the device.
Asthma Control Test Integration
Advanced sensors automatically prompt for monthly Childhood Asthma Control Test (cACT) or Asthma Control Test (ACT) scores, correlating them with sensor data to identify discrepancies. When cACT scores remain high despite poor adherence, this may indicate under-reporting of symptoms—a common pediatric phenomenon. Conversely, low control scores with perfect adherence suggest inadequate medication dosing or unaddressed triggers, prompting medication review rather than adherence lectures.
Environmental Trigger Correlation Analysis
Sensors that log GPS location and local air quality data can pinpoint specific triggers: the high pollen count at the soccer field, the classroom’s elevated CO2 levels, or grandma’s cat dander. Look for platforms that integrate with local school sensor networks or municipal air quality monitors. The most sophisticated systems now offer predictive alerts: “High tree pollen forecasted tomorrow—pre-treat before outdoor recess.” This transforms your child’s sensor from a diary into a proactive shield.
Age-Specific Considerations
One size fails all in pediatrics. Age-stratified features separate effective from frustrating sensors.
Toddlers (2-5): Simplification and Parental Overrides
For the youngest patients, sensors should be completely passive—no buttons, no screens, no required actions. Data flows automatically to parents, with AI filtering out false positives from rough play. Look for tamper-proof designs that can’t be removed by curious fingers. Parent dashboards should emphasize “dose delivered” confirmations rather than adherence percentages, reducing anxiety. Some platforms offer “parent simulation mode” where caregivers can practice technique with the sensor to ensure they’re coaching correctly.
School-Age Children (6-12): Building Independence
This developmental stage craves autonomy but needs scaffolding. Sensors with simple smiley-face feedback (green/yellow/red) teach self-monitoring without overwhelming detail. Peer comparison features should be avoided—they create stigma. Instead, look for “streak” celebrations and level-up systems that feel like educational apps. Parent dashboards should show adherence but withhold technique details, allowing children to self-correct without micromanagement. Integration with school health curricula, where nurses use sensor data for asthma education, reinforces positive behaviors.
Adolescents (13-17): Privacy and Self-Management
Teenagers demand sensors that don’t broadcast their condition. Ultra-slim, credit-card-sized devices that slide into inhaler pockets maintain discretion. Apps should offer teen-only modes where parents see only emergency alerts and weekly summaries, not daily blow-by-blows. Social features must be completely optional and private—no public leaderboards. Look for integration with teen health apps they already use, like fitness trackers, reframing asthma management as part of overall wellness. The most successful platforms offer teen-specific educational content about independence, driving, and college preparation with asthma.
Common Pitfalls and How to Avoid Them
Even well-intentioned sensor implementations fail. Recognizing traps prevents wasted investment and dashed hopes.
Over-Reliance on Technology
Sensors supplement, never replace, clinical judgment. Families who stop keeping action plans or skip appointments because “the sensor will catch everything” experience worse outcomes. Maintain your child’s written asthma action plan as the primary guide, using sensor data to inform decisions, not make them. Teach children to recognize symptoms independent of technology—sensors fail, batteries die, and emergencies happen offline. Schedule monthly “sensor-free” days where children practice self-management by feel, ensuring they don’t become helpless when technology falters.
Alert Fatigue in Busy Households
Too many notifications become background noise. Customize alert thresholds aggressively: set rescue inhaler alerts only for multiple uses within 24 hours, not single doses. Batch controller reminders into morning and evening digest notifications rather than per-dose pings. Use escalation logic—remind the child first, then parents only after non-compliance. The 2026 standard includes “quiet hours” that automatically suppress non-emergency alerts during school, sleep, or family time. If your family starts ignoring alerts, it’s time to recalibrate, not add more.
School Policy Conflicts
Many schools ban smartphone use during class, blocking sensor syncing and feedback. Proactively meet with school administrators before sensor deployment, providing documentation of medical necessity. Request written accommodation under Section 504 plans, explicitly permitting sensor app access during health office visits. Some districts now partner with sensor manufacturers for district-wide installations, providing secure school Wi-Fi networks for medical devices. If schools resist, choose sensors with offline modes that store data until home syncing, though this sacrifices real-time emergency alerts.
The Future of AI in Pediatric Asthma Sensors
2026 stands at the cusp of true artificial intelligence integration, moving beyond simple tracking to predictive intervention.
Predictive Exacerbation Alerts
Machine learning models now analyze weeks of technique quality, rescue inhaler frequency, and environmental data to predict exacerbations 48-72 hours before clinical symptoms. For children, this means pre-treating before the cough starts, potentially avoiding missed school and emergency visits. However, algorithms trained primarily on adult data may generate false positives for children. Look for platforms publishing pediatric-specific validation studies with positive predictive values above 80% for your child’s age group. The best systems learn your child’s unique patterns, reducing false alarms over time.
Personalized Medication Timing Algorithms
Circadian rhythm research reveals optimal medication timing varies by individual. AI-driven sensors analyze your child’s usage patterns, symptom timing, and inflammatory markers to suggest personalized dosing schedules—perhaps moving evening doses earlier for the child who experiences nocturnal symptoms despite perfect adherence. These algorithms must remain suggestions, not prescriptions, requiring clinician approval before implementation. The most ethical platforms provide transparency, showing families exactly which data points influenced timing recommendations.
Making the Final Decision: A Family-Centered Approach
After evaluating technical specs, return to your child’s unique needs and family dynamics.
Questions to Ask Your Pediatric Pulmonologist
Bring a checklist to appointments: Which sensors have you used with other patients? What integration does your clinic support? Are there age groups where you’ve seen better outcomes? What’s your protocol for reviewing sensor data—will you check it between visits? Do you receive alerts for concerning patterns? Their answers reveal whether a sensor will genuinely integrate into care or become orphan technology. If your clinician is unfamiliar with sensors, request a referral to a digital health-literate provider or asthma educator.
Trial Periods and Return Policies
Never commit without a 30-day trial. The best manufacturers offer money-back guarantees recognizing that pediatric adoption is unpredictable. Test during a typical month, not vacation or illness. Evaluate: Does your child actually use it? Do you check the app? Does it change any decisions? If the sensor sits unused after two weeks, return it—forcing technology rarely works. Some platforms offer “success-based” transitions where you rent for three months, then purchase only if adherence improves by a predetermined percentage, aligning financial risk with clinical benefit.
Frequently Asked Questions
Will a smart inhaler sensor replace my child’s peak flow meter?
While sensors provide more comprehensive data, they complement rather than replace peak flow meters. Peak flow objectively measures airway obstruction, while sensors track medication delivery and technique. Many clinicians recommend using both, especially during exacerbations or medication changes, as they measure different aspects of asthma control.
How do I convince my teenager to use a sensor without feeling stigmatized?
Choose ultra-discreet sensors that hide inside the inhaler and emphasize privacy features. Frame it as a tool for independence—“this lets you manage your asthma without Mom hovering.” Involve them in selection, prioritizing apps with teen-friendly interfaces. Never use sensor data punitively; instead, celebrate when they demonstrate self-management, reinforcing positive identity.
What happens if my child loses their inhaler with the sensor attached?
Most manufacturers offer loss protection programs for an additional monthly fee, providing discounted replacements. Immediately report loss through the app to deactivate the sensor and protect data. Some platforms include “last known location” features if the sensor was recently synced. For expensive sensors, consider homeowner’s insurance riders covering medical devices.
Can these sensors differentiate between rescue and controller inhaler use?
Yes, modern sensors recognize different inhaler profiles when properly configured. During setup, you’ll designate each inhaler’s medication type. Advanced sensors can even detect medication by analyzing actuation signatures, preventing data contamination if inhalers are swapped. This distinction is crucial for accurate adherence calculations and emergency alerts.
Are smart inhaler sensors waterproof enough for accidental washing machine trips?
IP67-rated sensors survive 30 minutes in 1 meter of water, covering most washing machine accidents. However, detergent exposure can damage seals over time. If washed, immediately remove the battery, rinse with fresh water, and dry thoroughly for 48 hours before use. Most warranties cover one water incident, but repeated exposure voids coverage.
How do sensors handle school inhalers that are shared among multiple students?
Shared school inhalers require multi-user sensors that can associate each actuation with the correct child via NFC badge tap or app confirmation. However, most experts recommend dedicated inhalers per child even at school to prevent cross-contamination and ensure medication availability. If sharing is unavoidable, choose sensors with rapid user-switching and strict data separation.
Will using a sensor affect my child’s insurance premiums?
Health insurers cannot legally raise premiums based on sensor data under the Affordable Care Act. However, life insurance applications may inquire about digital health device usage. Ethical sensor manufacturers include data use policies explicitly prohibiting sale to insurance underwriters. Always review privacy terms and consider sensors from companies that certify insurance neutrality.
What age should my child start using a smart inhaler sensor?
Sensors become beneficial once children use inhalers independently, typically around age 4-5 for simple rescue inhalers and age 6-7 for controllers requiring technique. For toddlers, passive sensors that track parental-administered doses help monitor caregiver adherence. The key isn’t age but developmental readiness—the child should understand the sensor is helping them breathe better, not playing a game.
How accurate are the environmental trigger features?
Environmental sensors achieve 85-90% accuracy for major pollutants (PM2.5, ozone) but struggle with specific allergens like pollen species unless integrated with local pollen counting stations. GPS-based location tracking improves accuracy but drains battery. Use environmental data as general guidance—“poor air quality day”—rather than definitive trigger identification, confirmed by symptom patterns over time.
Can my child use a smart inhaler sensor during sports activities?
Yes, but choose sensors with sport-specific modes that disable motion-based false actuation detection. Sweat resistance is crucial—look for IP68 ratings. Some sensors sync with fitness trackers to correlate exercise intensity with bronchodilator need, providing insights for pre-treatment timing. Ensure coaches understand the sensor is medical equipment, not a phone, exempting it from sports device bans.